Specific diseases
A pilot study of lifestyle modifications as prescribed in Āyurveda for diabetes mellitus type-II
Editor’s note
Diabetes mellitus is one of the commonest endocrine disorders affecting the entire biological system. Its incidence is increasing throughout the world due to changes in lifestyle and an increase of sedentary habits. Hence, lifestyle modifications are important in diabetes in controlling the blood-sugar level as well as preventing complications from this disease. Āyurveda, the ancient Indian medical system, gives a lot of importance to these issues which can be alleviated through āhāra and vihāra. A lifestyle module has been developed in this study by compiling the scattered information on āhāra and vihāra for madhumeha, an entity described in Āyurveda which resembles diabetes mellitus. This module was applied to 30 newly diagnosed diabetes patients for two months. The blood-sugar levels showed improvement at the end of the study.
Introduction
Diabetes is a global problem. WHO has projected that 346 million people worldwide have diabetes. In 2004, an estimated 3.4 million people died from consequences of high blood sugar. Deaths due to diabetes will double between 2005 and 2030. A healthy diet, regular physical activity, maintaining normal body weight and avoiding tobacco use can prevent or delay the onset of type II diabetes (1).The first line of therapy for a patient with suspected type-II diabetes involves advice about lifestyle modification, which includes āhāra (diet) and vihāra (routine activities and exercises). This can help to achieve adequate glycemic control in approximately 50% of patients; while anti-diabetic drugs will be required for 20-30% and insulin of the remainder (2).
Āyurveda is believed to be the first medical system in the world, which diagnosed and managed diabetes mellitus under the name, madhumeha. It is mainly caused due to apathya āhāra vihāra sevana (consuming of unwholesome food and lifestyle) (3). However if a person follows certain dietary rules, there is very little need for drug treatment. When a person is on an irregular diet, the drug treatment alone cannot control the disease (4).
Objectives of the study
1. Compiling the available literature on āhāra and vihāra
2. Developing āhāra-vihāra modules for diabetes mellitus type II
3. To evaluate the efficacy of the developed module.
Management of diabetes through āhāra and vihāra
ĀhāraFor a diabetic patient, a balanced diet which is low in fat, carbohydrates and cholesterol should be given always. The intake of food products which have kaṭu, tikta and kaṣāya tastes should be increased. In Āyurveda, bitter leaves and vegetables are recommended which are known for delayed absorption, thus causing a smaller increase of blood glucose after the meal. In Āyurveda, fibre-rich food like green vegetables and yava (barley) are highly recommended for a diabetic diet in different forms. The fibres get neither absorbed nor metabolised in the small intestine and so slow the movement of food and decrease blood glucose levels. The fibre content also supports the digestive system. Recent studies also suggest that the fibre content improves the ability of cells to receive and utilise insulin (5). Some examples of fibre-rich food are whole grams, the majority of fresh fruits, fresh vegetables, leafy vegetables, legumes, etc. In all the Āyurvedic classics, the groups of pathya āhāra dravyas (wholesome food) are described in detail and they comprise the entire food group noted in the following table:
Table 1: Pathya āhāra dravyas (6, 7, 8)
| Āhāra group |
Pathya āhāra (Sanskrit) | Latin name | English | Hindi |
| Śuka (Dhanya vargam) | Śāli | Oryja Sativa, Linn. | Rice | Chaval |
| Yava | Hordeum vulgare | Barley | Jeve, jan, jo | |
| Godhūvma | Tritium Sativa, Linn. | Wheat | Gehun | |
| Śyāmaka | Panicum frumentaceum | Barnyard millet | Saamva | |
| Kodrava | Paspalum scrobiculatum | Kodo millet | Kodova | |
| Vajrānna/sajja | Penniselumtypholeum | Pearl millet | Bajara | |
| Madhūlikā | Eleusine coracana | Indian millet | Makra | |
| Cūrṇa | Sorghum vulgare | Great millet | Jowar, jinor | |
| Kangu | Sertaria italica, Linn. | Italian millet | Kanguni | |
| Śimbi (Dhanya vargam) | Mudga | Phaseolus mungo, Linn. | Green gram | Pesalu |
| Caṇaka | Ciser arietinum | Bengal gram | Channa | |
| Kulutha | Dolichos biflorus, Linn. | Horse gram | Koolathee | |
| Adhaki | Cajanus indicus | Pigeon pea | Arahar | |
| Tikta śāka varga | Nimba | Azadirachta Indica | ||
| Karavella | Momordica charantia | Bitter gourd | Karela | |
| Medhika | Fenugrukum | Medhika | ||
| Guduchi patra | Tinospora cordifolia | Heart-leaved moon seed | Giloya | |
| Śaaka varga | Pattola | Trichosanthas anguina | Snake gourd | Chichonda |
| Kṣīya tumbi | Lagenaria siceraria | bottle gourd | Lauki | |
| Bimbi | Coccina grandis | Ivy gourd | Kanduru | |
| Lasuna | Aliun sativum | Garlic | Lasun | |
| Indravaruṇi | Citrullus colocynites | Bitter apple | Imdrayan | |
| Śatāvari | Asparagus racemosa | Flowers of a greenhouse | Shatavari | |
| Marica | Piper longum | Pepper | Kali mirchi | |
| Harita śāka varga | Culayī Tanduleyaka | Amaranthus spinosus | Spinach | palak |
| Vastukam | Chinopodium album | Goose foot | Chandanbetes | |
| Matsyākṣī | Alternanthera sessilis | |||
| Śigru patra | Moringo olifera | Horseradish | sahinjan | |
| Lavan-avarg | Saindhava lavaṇa | Rock salt | ||
| Phala varga | Jambu | Syzygium cumini | Blackberry | |
| Tāla phala | Borassus flabellifer | |||
| Śigru patra | Moringo olifera | Horseradish | sahinjan | |
| Kharjura | Phoenix sylvestris | Edible date | Pindakharjur | |
| Udumbara | Ficus glomerata | Country fig tree | Gular, aroa | |
| Aruku | Prunus communis Huds | Pear fruit | Alubhokar | |
| Kapita | Feronia elephantum | Elephant apple | Kavat | |
| Āmalakī | Emblica officinalis | Indian gooseberry | ||
| Bheeja (seeds) |
Kamala | Nelumbo nucifera | Kamala | |
| Utpala | Nymphoea Stellata | Indian blue water lily | Nilkamal | |
| Maṁsa (flesh) |
Hariṇa | Deer flesh | ||
| Śaśaka | Rabbit | |||
| Kapota | Pigeon | Kapot | ||
| Titira | Bird | |||
| Surā (Wine) | Old surā | Old wine | ||
| Taila (oils) | Sarsapa | Brassica Compestris | Mustard | Sarso |
| Tila | Sesamum indicum | Gingelly oil | Tel tel | |
| Ingudi | Balanitis aegypotiaca | |||
| Nikumba | Baliospernum montanum | Danti | ||
| Atasī | Linum usitatisimum |
Vihāra
Vihāra includes a daily regime of activities and exercises. Physical exercises increase the proportion of insulin-sensitive fibres in the muscles. They also increase oxidative enzyme activity, and both these changes favour the utilisation of fat as the fuel, thus controlling blood sugar elevations. Studies have shown that yoga produces significant results in the management of diabetes (9). A type-II diabetes mellitus patient should walk barefoot for 800 miles in a year (an average of 3.5 km/day) or do heavy work like digging a well or do exercises like wrestling, horse riding, vigorous walking, etc. However, thin people are advised to protect their strength and not to do vigorous exercises (10).
Materials and methods
This attempt was an observational study. No medicines were administered in this study. The prepared āhāra chart, vihāra A (Daily regimen — dinacaryā chart) and vihāra chart B (yoga) modules were given to the newly detected patients with diabetes mellitus type-II. Information on specific āhāra and vihāra practices were collected from Caraka Saṁhitā, Suśruta Saṁhitā, Aṣṭānga Hṛdaya and Sangraha, etc. classical textbooks and, based on that, the āhāra and vihāra modules were prepared for the convenience and need of present-day society. The choice of food items were based on local availability and the dietary pattern of the study population. In this study, samples of 30 patients were selected for the study.
Inclusion criteria
1. Patients of either sex, between the age group of 35-75 years
2. Patients with type–II diabetes mellitus
3. Patients with FBS >130 mg/dl & <180 mg/dl and PPBS >160mg/dl & <200 mg/dl
4. Newly detected type-II diabetes mellitus patients
5. Agreement to follow the prescribed āhāra and vihāra modules continuously for a period of 60 days.
Exclusion criteria
1. Patients with insulin-dependent diabetes mellitus type-I
2. Patients with fasting blood-sugar (FBC) >180 mg/dl and postprandial blood-sugar (PPBS) >200 mg/dl
3. Diabetic patients with any other complications
Diagnostic and assessment criteria
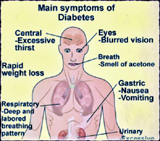
Diagnosis was based on the signs and symptoms of diabetes mellitus (polyphagia, polyuria, polydipsia) and where laboratory findings showed FBS >130 mg/dl and PPBS >160mg/dl. An assessment was done at the beginning, the 30th day, followed by a one month follow-up at the 60th day. Samples of urine, blood were collected three times from each patient for laboratory investigations of FBS, PPBS, and urine sugar at the beginning, on the 30th day and on the 60th day. All participants were given instruction sheets consisting of an āhāra chart, vihāra A (daily regimen – dinacaryā) chart and vihāra B Chart (yoga) for seven days. The patients were advised to repeat the modules for two months after the completion of each cycle. Patients were told to continue these with their regular medications, if any, for conditions such as hypertension, etc.
Table 2: Āhāra (diet) Chart (11, 12, 13)
Sunday |
Monday |
Tuesday |
Wednesday |
Thursday |
Friday |
Saturday |
|
Break- fast |
Broken barley upma + diluted milk(1:2) |
Broken wheat (dalia) + malt (barley churned drink ) |
Jowar saktu +malt (ragi churned drink) |
broken bajara Upma + diluted milk(1:2) |
Corn saktu + malt (barley churned drink) |
Boiled ragi powder bolus + diluted milk(1:2) |
|
Lunch |
Lentil soup + jackfruit vegetable cooked in mustard oil+chapatti of wheat + red rice (rakta śāli) |
Maize soup + Snake gourd vegetable cooked in mustard oil+ chapatti of barley+red rice(rakta śāli) |
Boiled barley soup + bottle gourd vegetable cooked in mustard oil + chapatti of jowar + red rice (rakta śāli) |
Vegetable soup+bitter gourd vegetable cooked in mustard oil+chapatti from ragi + red rice (rakta śāli) |
Ragi soup + spinach vegetable cooked in mustard oil + chapatti from maize+red rice (rakta śāli) |
Soup of green gram + jackfruit vegetable cooked in mustard oil + chapatti from bajara + red rice (rakta śāli) |
Boiled barley soup + Bottle gourd vegetable cooked in mustard oil+chapatti of jowar + red rice (rakta śāli) |
Evening Snacks |
Apupa (pancakes prepared with barley paste)+ tea |
Saktu (roasted corn flour) +diluted milk(1:2) |
Apupa (pancakes prepared with barley paste)+ tea |
Saktu (roasted corn flour)+ diluted milk(1:2) |
Apupa (pancakes prepared with barley paste)+ tea |
Saktu (roasted corn flour)+ diluted milk(1:2) |
Apupa (pan-cakes prepared with barley paste)+ tea |
Dinner |
Lentil Soup+ snake gourd vegetable cooked inmustard oil+ chapatti of barley |
Barley soup+ Jackfruit vegetable cooked in mustard oil+ chapatti of wheat |
Maize soup+ spinach vegetable cooked in mustard oil+chapatti of ragi |
Lentil soup + bitter gourd vegetable cooked in mustard oil+ chapatti of jowar |
Maize soup+ jackfruit vegetable cooked in mustard oil+ chapatti of maize |
Barley soup+ medhika vegetable cooked in mustard oil+ chapatti of wheat |
Vegetable soup+ bitter gourd vegetable cooked in mustard oil+ chapatti of barley |
Table 3: Vihāra chart A (daily regimen — dinacaryā) (14, 15)
Time |
Type of Vihāra |
5.30am- 6.00am |
Wake up and morning ablutions |
6.00am-6.30am |
Morning walk |
6.30am-7.30am |
Special yoga techniques for diabetes mellitus |
7.30am-8.00am |
Bath and getting fresh |
8.00-am-8.30am |
Pūja (bhakti yoga) |
8.30am-9.00am |
Breakfast |
9.00am-1.00pm |
Office work/Housework/karmayoga |
1.00pm-2.00pm |
Lunch |
2.00pm-2.30pm |
Normal walking/deep relaxation techniques |
2.30pm-4.30pm |
Office work/housework/karmayoga |
4.30pm-5.00pm |
Snacks and tea |
5.00pm-6.00pm |
Office work/housework/karmayoga |
6.00pm-7.00pm |
Evening walk |
7.00pm-7.30pm |
Getting fresh |
7.30pm-8.30pm |
Dinner |
8.30pm-9.30pm |
Book reading |
9.30pm-10.00pm |
Going to bed |
Table 4: Vihāra chart B (yoga) (16, 17)
Day |
Type of yoga |
| Monday | Sūryanamaskāras (set of 12 aasanas), prāṇāyama, deep relaxation techniques |
| Tuesday | Asanas, prannayama, meditation |
| Wednesday | Sūryanamaskāras, praannaayama, deep relaxation techniques |
| Thursday | Asanas, praannaayama, meditation |
| Friday | Sūryanamaskāras, praannaayama, deep relaxation techniques |
| Saturday | Asanas, praannaayama, meditation |
| Sunday | Sūryanamaskāras, praannaayama, deep relaxation techniques |
Result
In these studies, 30 patients were tested for urine sugar, FBS and PPBS. Out of the 30 samples, 23 results came down to normal levels. In the other seven samples, urine sugar came to nil and their FBS and PPBS levels decreased from before.
Discussion and conclusion
These patients were not given any medicines related to diabetes mellitus. Approximately 73% patients achieved FBS of < 130 mg/dL or PPBS < 160 mg/dL at the end of the study, the remaining 27% of patients showed decreased levels of FBS, PPBS. Reasons for that might be an inability to follow prescribed āhāra and vihāra, apathya-āhāra-vihāra sevana. A larger group is required to prove results conclusively. Thus the pilot study is an attempt to take in all the traditional wisdom prescribed in our ancient texts for the management of DM type-II. As per the principle indicated by the bṛhatrayis and laghutrayis of Āyurveda, these developed modules are well suited for controlling the urine and blood-sugar levels in diabetes mellitus type-II.
References
1. Diabetes, World Health Organization http://www.who.int/mediacentre/factsheets/fs312/en/index.html(Accessed 2nd June 2013).
2. Gupta A, Byadgi PS. Critical Appraisal of Medical Nutrition Therapy In Ayurveda For Diabetes Mellitus, International Journal of Medical and Pharmaceutical Sciences 201; 2(2): 6-11.
3. Agnivesha. Caraka Saṁhitā (Chakrapanidatta commentary), Vol. 3. Sharma RK, Bhagavandash, (eds.) Varanasi: Chowkamba Sanskrit Series; 2010. Cikitsā Sthana 6/18-21. p.304.
4, Lolimbaraja. ‘Sudha’ hindi teekayukta, Vaidya jeevanam. 3rd ed. Varanasi: Chawkhambha Sanskrit Series; 1965, p. 4.
5. Goli Penchala Prasad, Babu G, Swamy GK. Contemporary Scientific Support on Role of Ancient Ayurvedic Diet and Concepts in Diabetes Mellitus (Madhumeha), Ancient Science of Life June 2006; 25 (3 & 4): 84-91.
6. Vagbhata. Aṣṭanga Sangraha. 9th ed. K. R. Srikantha Murthy KR. (ed.) Varanasi: Chaukhambha Orientalia; 2005, Sutra sthana, 7th chapter, p.115-64.
7. Agnivesha. Caraka Saṁhitā (Chakrapanidatta commentary), Vol. 3. Sharma RK, Bhaga-vandash, (eds.) Varanasi: Chowkamba Sanskrit Series; 2010, Cikitsā Sthana 6/18-21, 46-48, p.304, 311.
8. Susruta. Suśruta Saṁhitā (Drudabala commentary). Varanasi: Chawkhambha Sanskrit Series; 2010. Cikitsā Sthana, 11/6, 11 & 12. p. 384, p. 387.
9. Yadav RK, Ray RB, Vempati R, Bijlani RL. Effect of a comprehensive Yoga based lifestyle modification programme on lipid peroxidation. Ind J Physiol Pharmacol 2005; 49: 358-62.
10. Suśruta. Suśruta Saṁhitā (Drudabala commentary). Varanasi: Chawkhambha Sanskrit Series; 2010. Cikitsā Sthana, 11/11-12, p.387.
11. Agnivesha. Caraka Saṁhitā (Chakrapanidatta commentary), Vol. 3. Sharma RK, Bhaga-vandash, (eds.). Varanasi: Chowkamba Sanskrit Series; 2010, Cikitsā Sthana 6/18-24, 46-48, pp.304-5, 311.
12. Bhisagratna, Bhavprakasha of Sri Bhavamishra. Varanasi: Chawkhambha Sanskrit Bhavan; 2009, pp. 38-41.
13. Suśruta. Suśruta Saṁhitā (Drudabala commentary). Varanasi: Chawkhambha Sanskrit Series; 2010. Cikitsā Sthanaa, 11/4-5, pp. 383-4.
14. Agnivesha. Caraka Saṁhitā (Chakrapanidatta commentary), Vol.3. Sharma RK, Bhaga-vandash, (eds.). Varanasi: Chowkamba Sanskrit Series; 2010, Cikitsā Sthana 6/50, p.312.
15. Vagbhata. Aṣṭanga Sangrah. 9th ed. Srikantha Murthy KR. (ed.). Varanasi: Chaukhambha Orientalia; 2005, Sūtra sthana, 3rd Chapter, pp.31-56.
16. http://www.yogaindailylife.org/esystem/yoga/en/192600/asana-and-exercise-categories-according-to-benefits/asanas- and-exercises-to-activate-the-pancreas-for-diabetes (Accessed 20th July 2013).
17. http://www.ayurveddoctor.com/yogasanas-for-diabetes.html(Accessed 29th July 2013).
Dr. Goverdhanam Vani is Āyurvedic Physician and Research Scholar and Dr. J.S.R.A. Prasad is Asst. Professor at the Dept. of Sanskrit Studies, University of Hyderabad.
Share with us (Comments, contributions, opinions)
When reproducing this feature, please credit NAMAH, and give the byline. Please send us cuttings.